Carefully Selected Experts, Trusted Institutions
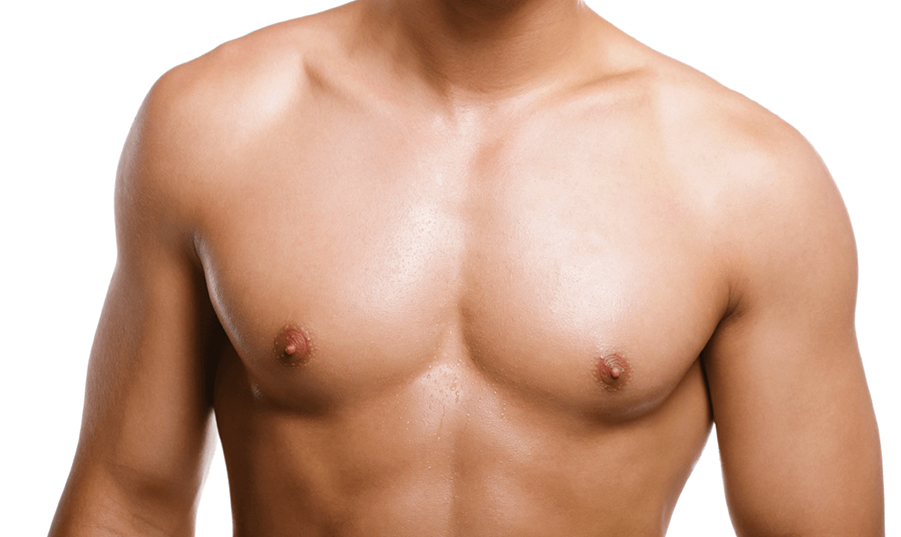
The occurrence of gynecomastia is quite prevalent globally, including in cities like Istanbul, with a significant number of adolescent males experiencing this during puberty—estimates suggest that up to 70% of boys may develop some degree of gynecomastia during this transitional phase. Despite its frequency, the condition often resolves spontaneously, with about three-quarters of cases returning to normal without medical intervention within a couple of years.
While gynecomastia is not typically associated with serious physical health risks, the impact on emotional and mental well-being should not be underestimated. Young men and boys may face psychological distress or social challenges such as teasing or bullying due to the physical changes they undergo. Consequently, even in the absence of physical health concerns, treatment might be sought to alleviate the psychological and social distress associated with the condition.
For persistent cases of gynecomastia, especially those that do not recede over time, medical evaluation is advised. Treatment options vary depending on the severity and persistence of the condition, with surgery being a viable option for those seeking to remove excess breast tissue and restore a more traditional male chest contour. This surgical solution can play a crucial role in improving self-esteem and quality of life for individuals affected by gynecomastia.
The development of gynecomastia is often linked to fluctuations in hormonal levels, specifically the imbalance between estrogen and testosterone in the male body. While testosterone is recognized as the primary male sex hormone, men also naturally produce estrogen in smaller quantities. Estrogen is traditionally considered a female hormone, but in males, it plays a role in modulating libido, erectile function, and the production of sperm.
When there is a reduction in the levels of testosterone or an elevation in the levels of estrogen, the balance can tip, potentially leading to the growth of breast tissue characteristic of gynecomastia. Various factors can contribute to such hormonal imbalances:
Aging: As men age, their testosterone levels naturally decline, while body fat, which can convert testosterone into estrogen, tends to increase, possibly leading to gynecomastia in older men.
Puberty: Hormonal levels can fluctuate significantly during puberty, and temporary imbalances can result in the development of breast tissue in young males, which typically normalizes over time.
Medical Conditions: Certain health issues, such as hyperthyroidism, kidney failure, or liver disease, can alter hormone levels and increase the risk of developing gynecomastia.
Medications: Some drugs are known to affect hormonal balance. These can include steroids, medications for hypertension, antipsychotics, and anti-ulcer drugs, among others.
Substance Use: The use of alcohol, marijuana, heroin, and amphetamines has been associated with gynecomastia, as they may potentially disrupt normal hormonal regulation.
Moreover, certain personal care products, foods, or environmental factors that contain estrogenic compounds could contribute to the hormonal changes leading to gynecomastia. It is important for individuals experiencing breast tissue enlargement to seek medical advice to determine the underlying cause and appropriate treatment, if necessary. Addressing the root cause can often lead to an improvement in the condition without the need for surgical intervention.
Gynecomastia presents with distinct physical manifestations, often affecting one or both breasts asymmetrically. Notable signs include:
It is important to differentiate between true gynecomastia and a similar condition known as pseudogynecomastia. The latter involves the accumulation of fatty tissue in the chest area rather than the growth of glandular breast tissue. Pseudogynecomastia is closely associated with overweight or obesity and can often be alleviated through weight loss practices such as improved diet and increased physical activity.
Although the symptoms of gynecomastia can be similar to those of breast cancer, it is important to note that male breast cancer is quite rare. Nonetheless, the overlap in symptoms underscores the importance of seeking a professional medical evaluation for any significant changes in breast tissue.
An accurate diagnosis often involves a physical examination and, if necessary, further tests such as blood analyses, imaging studies, or tissue biopsies. By consulting with a healthcare provider, individuals can ensure that they receive proper guidance, and if needed, effective treatment tailored to the specifics of their condition.
Surgical intervention can be considered for individuals with gynecomastia, particularly when medicinal treatments fail to yield results. Surgery is renowned for its effectiveness in resolving the condition, offering a permanent alteration of the chest contour by excising superfluous breast tissue.
Performing surgery on patients who have not yet passed through puberty is generally discouraged because of the potential for the breast tissue to grow back. Postponement until adulthood, when hormonal levels have stabilized, is usually recommended.
There are two primary surgical procedures employed to correct gynecomastia:
Reduction Mammaplasty: This surgery is suited for cases with a significant glandular tissue component. The procedure involves the removal of the glandular tissue and excess skin, often accompanied by contouring of the chest to achieve a more traditionally masculine appearance.
Liposuction: This technique is predominantly effective for removing fatty tissue and is chosen when pseudogynecomastia is diagnosed, or in cases where the fatty component of breast enlargement is prominent. Liposuction involves inserting a cannula, a small, thin tube, through minor incisions, using it to loosen excess fat, which is then aspirated from the body.
The risks associated with these surgical procedures, while typically low, are nonetheless present and include potential anesthesia complications, hematoma (blood clot) formation, persistent pain, asymmetry in the contour of the chest, infection at the incision sites, and scarring.
Patients considering surgery for gynecomastia should engage in a thorough discussion with their surgeon to understand the benefits, risks, and what to expect during recovery. A clear understanding of the surgical process and its aftermath will contribute to making an informed decision that aligns with the individual’s health considerations and aesthetic goals.
Recovery after gynecomastia surgery, also known as male breast reduction, is an important phase where the body heals and adapts to changes. Here’s a general overview of what one can expect postoperatively and some tips for a smooth recovery:
Immediate Post-Operative Phase
First Few Weeks
Long-term Recovery
Monitoring and Follow-up
Lifestyle Adjustments
Emotional and Psychological Aspects
Final Results
Each patient’s recovery process is unique, and it’s crucial to follow the personalized care plan provided by your healthcare provider. Remember to keep all scheduled post-operative appointments and communicate openly with your surgical team about any concerns during your recovery.



